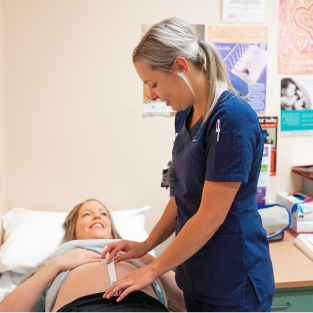
Key Achievements
In 2020-21, the Clinical Excellence Commission:
- Supported 1.5 million webpage views and over 250,000 downloads of COVID-19 resources in 2020-21.
- Collaborated with HealthShare NSW to conduct 197 personal protective equipment (PPE) reviews, totalling 430 PPE product assessments, and delivered weekly PPE audits via the Quality Audit Reporting System for local health districts and specialty health networks.
- Responded to 968 notifications regarding issues with medical devices, medicines and biological agents with our Critical Response Unit conducting risk assessments. Of these, 18 required system-wide critical responses related to product issues and shortages to ensure the safe delivery of care and continued service delivery. We issued 25 urgent safety alert broadcasts, including 12 related to clinical issues and 13 related to medicines and vaccines. These were in addition to 19 medication safety updates and 10 medication safety communications as part of our primary function to minimise potential harm.
- Developed and led implementation of a statewide Respiratory Protection Program with participation by more than 106,520 health workers; and coordinated a whole-of-health approach to developing standardised resources for fit checking, fit testing, reporting and training.
- Developed new Morbidity and Mortality meeting guidelines in conjunction with clinicians and established these on the Quality Improvement Data System platform for clinical teams to access near real-time data and generate insights for meetings. The new Morbidity and Mortality guidelines identify six core principles that reflect contemporary safety and quality principles, which are guided by Human Factors science to support robust processes that improve learning and system improvement.
- Developed, tested and released a Safety Culture Measurement Toolkit to serve as a self-contained set of instructions and templates to enable health services to administer a safety culture survey effectively and adapt for local conditions.
- Developed the Safety Fundamentals for Person Centred Communication tools to support staff in building relationships and partnering with patients, their families and carers in decision making. They include Teach Back, What Matters to You? and the Patient Delivered Handover.
- Implemented the revised NSW Health Incident Management Policy following the commencement of legislative changes for serious incident management in December 2020. Collaborated with eHealth NSW to align the use of the incident management system platform through refocusing process aims to improve reliability, quality, timeliness, strength of incident management, responses to review recommendations and system learning. Supported local health districts and specialty health networks to implement the use of the Preliminary Risk Assessment and serious adverse event review methodologies by hosting 36 masterclass sessions for 1507 participants prior to commencement of legislation; developing 80 resources including templates, toolkits, workbooks, fact sheets and explainer videos; and hosting two Patient Safety Manager Forums following implementation attended by 195 staff.
- Developed the updated Safety & Quality Essentials Pathway that learns from and replaces the Foundational Clinical Leadership and Executive Clinical Leadership Programs. The pathways aim to build the skills and knowledge needed of effective leaders for safety and quality improvement in daily practice. The CEC Academy works with health entities through partnership agreements to support sustainable local implementation.
- Partnered on 15 research projects to support innovation and translation in a range of quality and safety priorities, including stillbirth prevention, falls prevention, antimicrobial stewardship and virtual clinical pharmacy services.
New CEC Academy

Ken Hampson (former Director of Clinical Governance), left, and Amanda Larkin (Chief Executive, SWSLHD), right
Learning together for safety and quality
The CEC Academy brings people together to learn, share and apply the principles of safety and quality improvement in clinical practice.
In 2020/21, the Academy made substantial progress by working with local health entities to review and update its safety and quality capability development programs.
The goal is to establish a pathway for all staff that grows their awareness, understanding and practical application of safety and quality improvement in daily practice.
Working with local health entities, the CEC developed the Safety & Quality Essentials Pathway as one strategy to build capability across the NSW Health workforce in patient safety and quality improvement.
The Pathway contributes to reducing harm by offering tailored development through programs aligned to the Healthcare Safety and Quality Capabilities set.
Foundational is the first level of the Pathway and is designed for all NSW Health employees. From January to June 2021, 6,586 NSW Health staff have already completed all Foundational modules, and 8,230 had completed the 6 Dimensions of Healthcare Safety & Quality video.
Leading from the Chief Executive's office, South Western Sydney Local Health District (SWSLHD) has been a key driver to the impressive uptake of the Foundational programs within the Pathway.
Amanda Larkin (Chief Executive) and Ken Hampson (former Director of Clinical Governance) were among the first people to complete the Foundational program and have made it a requirement for all SWSLHD employees.
At the opposite end of the pathway, the Academy continued to partner with SWSLHD for the first test of the Applied Safety & Quality Program with 12 local leaders in safety and quality.
The Applied Safety & Quality Program is a 12-month development opportunity designed for local leaders of safety and quality with a focus on workplace application to build local capability and lead continuous improvement.
Quotes from SWSLHD Applied SQ Program participants:
"My most valuable learning was that Improvement Science is adaptable to the dynamic nature of organisational and patient safety requirements. My own thinking also needs to be adaptable and dynamic."
"I now have a lot of resources to build my repertoire of change management, and hopefully I can support more staff through driving their own change projects."
Reflecting on learnings so far, the CEC has committed to work with local health entities through implementation partnerships over the next two years. The goal is to build from the foundations up, to the point where all pathway programs can be sustainably locally delivered and integrated with local strategic priorities.
Morbidity & Mortality

M&Ms - New Guidelines
Traditionally Morbidity & Mortality (M&M) meetings have not focussed on education or felt like a 'safe space' to share information from which to learn, improve care and build team cohesion.
To provide guidance on how to lead and facilitate safe and meaningful discussions within the M&M, the CEC consulted and collaborated with clinicians to develop the new M&M meeting guidelines.
The new M&M guidelines identify six core principles that reflect contemporary safety and quality principles, which are guided by Human Factors science to support robust processes that improve learning and system improvement. These principles allow health agencies to review the quality of the care that is being provided to their patients and to identify any opportunities for improvement.
A key aspect of effective M&M meetings is having access to meaningful patient level data to support the M&M process. The CEC has developed an M&M Module in the Quality Improvement Data System (QIDS) that provides clinicians with access to local Hospital Acquired Complication (HAC) data from the Health Information Exchange (HIE), ims+, and other sources. By making it easy to review this data at the Local Health District, hospital and ward levels, opportunities for improvement can be identified.
To enable LHDs to run effective M&M meetings, supporting resources developed by the CEC include cue cards for presenters and a checklist for M&M meeting chairs.
The CEC has also collaborated with clinicians in publishing its first educational podcast series on M&Ms, further raising awareness of the important change in how M&M meetings are being approached. Described by some as a masterclass in how to undertake M&M discussions in a safe space for learning and improvement, these podcasts set the bar for how best to manage these vital meetings.
Quotes from the podcast participants:
"Using the structure of the CEC guidelines for the M&Ms, we've actually developed a very structured way in which we approach every meeting….. And then we use the CEC M&M template for reporting and everyone's used to seeing that."
Dr Andrea Christoff, Medical Co-Director, MD FCICM FRACP
"...the number one thing is - and it's beautiful to see it on the guidelines from the CEC - the safety of the people who are actually at the meeting…… We're missing the opportunity of focusing on learning from what we did well. It is so important….I was so happy to see the CEC's guidelines talking a lot more about Safety II introducing those ideas."
Dr Dane Chalkley, Deputy Director WellMD Centre, SLHD Emergency Department, Senior Staff Specialist in Emergency Medicine, RPAH BSc. (Hons) MBBS FRCEM FACEM
"...really important to me to choose the cases that we talked about really carefully. So, only choose the cases where you're actually going to learn from them, not where you're just going to embarrass or shame someone…. You don't learn if you're feeling ashamed and you don't learn if you're feeling frightened…"
Dr Clare Skinner, Staff Specialist in Emergency Medicine, Hornsby Ku-ring-gai Hospital BSc BA(Hons) MBBS MPH FACEM.
COVID-19
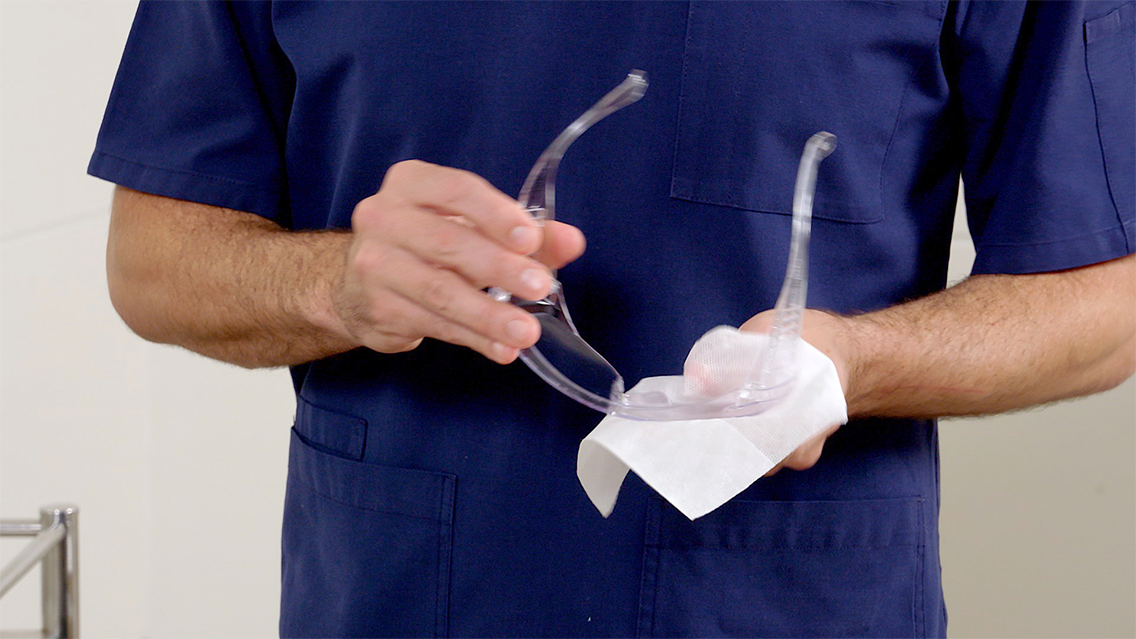
COVID-19 Infection Prevention and Control response
With the declaration of a pandemic on 11 March 2020, under NSW legislation, the CEC became the lead agency for Infection Prevention and Control (IPAC) in NSW.
Under the leadership of Chief Advisor Kathy Dempsey, CEC's Healthcare Associated Infection (HAI) and Infection Prevention and Control (IPC) team developed a comprehensive range of COVID-19 IPAC resources setting clear clinical guidelines for the NSW Health community.
The IPAC team influenced IPAC compliant behaviour across the health system through webinars, support sessions, and educational videos. The cornerstone of the HAI team's approach was the creation of the COVID-19 IPAC Manual, a consolidated 215-page guide for acute and non-acute healthcare settings. The manual is regularly updated and provides healthcare workers with guidance on COVID-19 infection prevention and control requirements for the management of patients or clients with suspected, probable or confirmed COVID-19.
To ensure the consistent application of processes and procedures, the team initiated new channels of communication to share knowledge with NSW clinical Communities of Practice and to Infection Control Practitioners networks across the NSW Health system, LHDs, enabling them to respond to the pandemic challenge. The team also developed and led implementation of a state-wide Respiratory Protection Program (RPP) with participation by more than 100,000 health workers.
The team also coordinated a whole of health approach to developing standardised resources for fit checking, fit testing, reporting and training. In addition, the team implemented robust governance processes for Personal Protective Equipment (PPE) and developed a range of downloadable PPE instructional videos to embed safety protocols.
The success of the team's COVID-19 response strategy was evident in the 1.5 million webpage views and 250,000 downloads of CEC's COVID-19 infection prevention and control resources.
As new needs emerged, the team assisted Residential Aged Care Facilities, educational facilities, multi-purpose services, private hospitals, community residential care group homes, hostels and refuges.
The team's vital work with NSW Hotel Quarantine and Airport Program Quality Assurance Program contributed substantially to key outcomes in the successful control of COVID-19 in NSW by helping prevent the spread of the virus into the wider community from any arriving travellers.
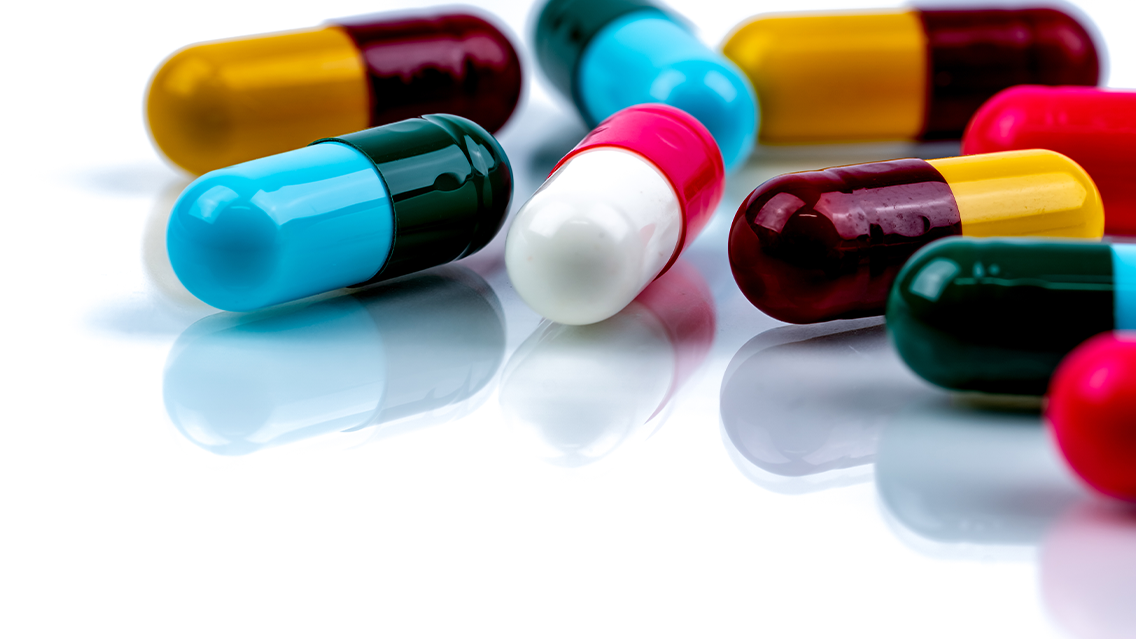
Maintaining medication supply during COVID-19
A significant challenge for NSW Health during the COVID-19 pandemic has been ensuring adequate supply of essential medications for all facilities due to global medication shortages and supply chain constraints. As the lead agency for critical response to all COVID-19 medication supply and safety issues, the CEC Medication Safety Team (MST) has focused on ensuring that medicines are available to treat all patients and when alternatives are recommended for use in our facilities, that they do not introduce safety concerns.
The CEC MST have liaised with other NSW Health agencies to ensure safety in the continuous supply of medication being used in our facilities. All alternative products undergo rigorous review to ensure they do not introduce risks that could lead to prescribing, dispensing or administration errors e.g., packaging variations and/or differing storage requirements.
In the 2020-2021 financial year,
- 571 supply issues were made apparent to the CEC requiring investigation for potential safety issues
- 123 of these were reported to frontline staff due to safety risk(s) requiring local mitigation
- 17 resulted in a formal safety communication (including a Safety Alert Broadcasts in some instances)
To summarise the emerging safety risks requiring local mitigation, the CEC MST created a Medication Safety Update document that was disseminated to the system regularly (weekly initially and then fortnightly) until early November 2020 when it was transitioned to a webpage hosted on the CEC website.
To understand the utility and timeliness of the initial updates, consultation was undertaken through interviews with six Pharmacy departments and an electronic survey was disseminated to NSW Health employees. Overall, the feedback was positive with respondents agreeing that the updates contained valuable and relevant information. Comments regarding the timeliness and format of the update led to a transition to a dynamic online format with the ability to filter and sort entries. Up-to-date information is now added as it becomes available, and clinicians are alerted to changes via email (if they choose to join the subscriber list). Additionally, a document summarising the last month's medication safety and supply related issues is now released at the beginning of each month (e.g. June 2021 update) and can be used by frontline clinicians to table at relevant committee meetings, such as Drug and Therapeutics Committee meetings.
The CEC has demonstrated agility in their response to medication supply and safety during the pandemic to meet frontline needs. Collaboration across NSW Health agencies resulted in a central reference point which could be relied upon as the 'source of truth' for up to date information. This is unprecedented and has broken down barriers to allow for a more efficient and effective process.

CEC coaches Thulasee Sri Ganeshan, Ingrid Hutchinson, Mary Fullick and Kate Roper
Redesigning Quality Improvement Toolkits
The CEC Quality Improvement Toolkits support local healthcare teams to start and sustain a quality improvement (QI) project focusing on clinical areas where the risk of harm is well recognised.
Design, consultation phase and improvements to the toolkits
The redevelopment and standardisation of the CEC toolkits consisted of two rounds of consultation via the Quality Audit Reporting System (QARS) survey and email correspondence targeting a wide range of clinicians and managers across NSW. Over 50 survey responses and 15 individual experts' feedback were received. As a result, the following improvements to the design of the toolkits were implemented:
- Human centered design with interactive layout and resources specific to each clinical area
- Step by step approach to Improvement Science allowing anyone to conduct a project with ease
- Initiation of Communities of Practice (CoPs) providing a channel for clinicians to reach out for advice and to share their own learning across NSW health facilities
- Formation of the CEC toolkit working group to guide standardised toolkit development and maintenance.
Official launch and introducing the Communities of Practice (CoPs)
The CEC launched six QI toolkits in June 2021 (with plans to launch at least another six in the coming year). Communication strategies included an introduction video by Chief Executive Carrie Marr, a series of webinars and advertisements through specific clinical networks. The strategies were well received by our colleagues, with over 500 staff across NSW registering for three webinars.
Within three months of the launch, the toolkit webpages had over 4,500 views and 100 individual CoP registrations. This includes enquiries from other States finding the toolkits very useful.
Positive feedback from clinicians
Here are some specific feedbacks from clinicians who have reviewed and/or used the toolkits.
"Thanks CEC for developing a practical and useful toolkit which is simple to follow and step-by-step guide. I love the examples to illustrate the point and helps my understanding."
Angela Wai, Senior Pharmacist Medication Safety, SLHD.
"I found the information very helpful, VTE Prevention and improving the use of the VTE risk assessment has been a project we have been looking at for a number of years. The driver diagram was useful to compare with our project's driver diagram."
Maria Pron, Quality and Accreditation Manager, Fairfield Hospital.
Our thanks
In the preparation of this document we would like to thank management, clinical staff and communications teams in the following local health districts: Nepean Blue Mountains, Northern NSW, Northern Sydney, Sydney, and South West Sydney.